Login
Register
Login
Register



The objective of this course is to explain the different types of loading protocols that exist in oral implantology and what criteria apply to them.
Presented by: Raquel Zita Gomes
Event Date: April 23, 2024
View Details
FROM THE FORUM
View DXP Forum
LIVE EVENTS
View All Events
NEW CONTENT
View All Content
- 3/21/2024
IV Sedation and When to Introduce an Anesthesiologist
- 1/26/2024
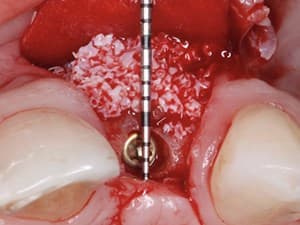
When considering implant therapy in the esthetic zone, replicating the natural soft tissue frame may present challenges for the treating clinician. This present...
OUR CONTINUING DENTAL EDUCATION SPECIALTIES
TRY BEFORE YOU BUY
Using a Flexitime® Matrix in Anterior Composite Restorations
Feb 17, 2010
Proof of Principle: human histologic demonstration of socket healing with socket shield and grafting using non-demineralized autologous tooth dentin graft
Apr 24, 2023
The Replacement of Small-Diameter Teeth in the Esthetic Zone Using Narrow-Diameter Implants
Sep 20, 2022
4 Steps to a Predictable Full Arch Rehabilitation
Jun 1, 2021
ATTEND EVENTS WORLDWIDE

Date: 5/16/2024
Location: Modena, Italy